As your medical organization expands, so do its financial operations. Instead of trying to keep all bills, claims, and payments under control, you should focus on providing the best services to patients instead.
Cloud-based healthcare billing solutions and medical claim processing software help healthcare organizations like yours increase revenue and reduce the cost of insurance claims and patient payment management. The software can be integrated into your existing system or developed from scratch—both options are viable. We know this because Demigos has been developing medical billing systems for years.
Continue reading to discover how cloud-based medical billing software can streamline your processes, what its features and requirements are, how does it work, and how much implementing it costs.
Why you need a custom medical billing software
Creating custom medical coding and billing software can help healthcare organizations increase their revenue and reduce the costs of managing insurance claims and payments. Well-designed medical billing software provides a seamless billing process, manages and tracks all payment information, sends medical claims automatically and on time, and reminds patients about payment or insurance expiration.
Read also: Guide on Developing a Health Insurance Application
Let’s focus on each benefit of developing a medical billing application individually:
Reduced overall cost of medical bills
Administrative costs are responsible for 25% of all healthcare spending. The portion of billing and insurance-related functions in this percentage varies:
-
8% for private insurers
-
14% for physician offices
-
11% for hospitals.
Implementing medical billing software can help reduce these numbers and improve revenue cycle management. Improved processes account for effective operations, while less paperwork and less staff mean smaller overheads.

Decreased human error
In a hospital environment, even minor errors can be dangerous, leading to reputational or financial losses. But when many processes in a clinic are carried out manually, there will definitely be errors. Since machines aren’t as prone to mistakes as people, with billing software, human errors go down while the claims management efficiency goes up.
Improved information security
Keeping your patient and financial information on a secure server in the cloud is safer than storing piles of documents with sensitive information anyone can read. A database only several high-level administrators have access to is a secure location for storing patient billing addresses, personally identifiable information, insurance details, scans, and test results, and more.
How does modern medical claims processing software work?
Find below a healthcare claims processing software workflow
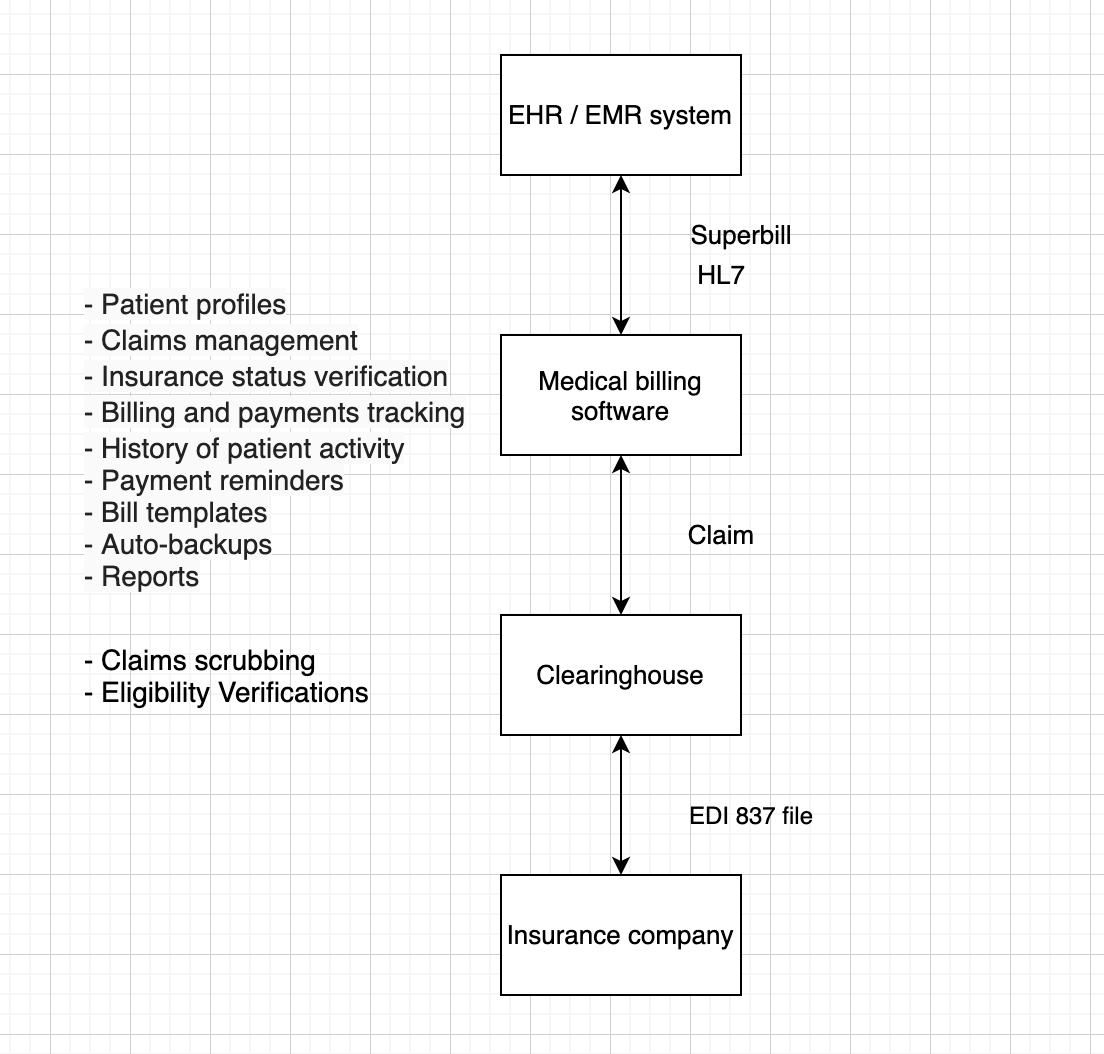
-
EHR/EMR sends a superbill that lists all the services provided to the client. Each service is aligned with a CPT code, each diagnosis with an ICD-10 code. Typically, the superbill is sent in an HL7 format.
-
After that, the superbill goes to the billing management system. The system checks the patient’s insurance plan and, being integrated with EHR, verifies the validity of the information submitted. This data forms the basis for a claim. Given that different insurance companies cover different services, there are different claims formed within a single superbill.
-
Next, these claims are sent over to the clearinghouse. The task of a medical billing clearinghouse is to ‘pack’ the claim into a format accepted by the insurance company. The EDI 837 file format is the most typical. There’s a catch, though: the healthcare provider and the insurance company might have different clearinghouses. If that’s the case, the healthcare provider’s clearinghouse has to send a claim to the insurance company’s clearinghouse that will, in turn, provide the insurance company with the file in the required format. The government dictates some regulatory requirements for this file format, so it’s essential to know all the nuances.
-
Finally, the insurance company gets the claim in the necessary format. If there are any questions or comments, the process runs all the way back. The insurance company sends a message in the same format back to the clearinghouse that had sent the claim. The clearinghouse goes back to the billing management system, and so on. That’s why it takes a while for all these transactions and approvals to come through. With two clearinghouses in one chain, delays are simply inevitable.
Read also the article about medical billing trends.
The must-have medical billing software features

Three of the critical features of medical billing and claim processing software should perform flawlessly are billing, claim management (transmission, retrieval, processing, and submission), and medical coding. Let’s look at them in detail.
Claims processing and financial management
If your medical billing solution has this feature, it means the software will automatically send and receive claims (including resubmissions), code, and charge entry. This also includes:
-
Supplying remittance advice when a bill is paid
-
Claims scrubbing
-
Carrying out dunning management
-
Compliance tracking
Patient billing
Your software should bill clients, process and track payments, keep invoice and payment activity history and all related billing information about appointments and treatments received. Offering and storing templates for a variety of billing transactions is also a handy feature.
Additionally, the billing software should send out automatic reminders to patients, reminding them of unpaid bills or insurance expiration. Monitoring all that manually would be a huge time killer.
Automated insurance verification
Some healthcare facilities have a person or an entire department where dedicated people verify if patients have the necessary insurance coverage. This includes both scheduled and walk-in patients, and when a person comes in without an appointment, they additionally need to wait for their health insurance information to be checked.
Read also: How to Develop Health Insurance Software
The medical billing software you’re going to use in your healthcare facility should handle insurance verification automatically. This will speed up patient admission, decrease the denial rate, and leave more time for actual patient care. So, make sure this software integrates with insurance carrier networks.
Secure data and patient information storage
Your medical billing software should store (locally or in the cloud) confidential data like patient personal information, insurance details, billing and bank information, medical records, allergies, medications, transaction history, etc. Having the necessary information beforehand cuts down routine personal communication, increasing patient satisfaction and improving admission time.
That said, the data storage should be secure and comply with the HIPAA or GDPR standards. Keeping up with data compliance in different countries or states is challenging but critical, so make sure the vendor you are working with knows the ins and outs of healthcare information security. Automatic backups should also be a must.
Reporting
It would also be nice to have the system provide you with reports on the performed actions. Gathered neatly in a dashboard, these financial, staff, and patient reports will help you analyze operations and see what aspects need improvement.
See also how we developed an on-demand nurse staffing platform and details of home care scheduling software development.
Integrating custom medical billing software into an existing EHR
Electronic health records (EHR) represent a huge improvement over traditional paperwork procedures, opening new opportunities for healthcare providers. By interacting with other medical processes, EHR creates a more comprehensive view of the patients' medical information. Modern EHRs organize and prioritize practice workflows and help health providers reduce mistakes, especially when prescribing medication.

Modern medical billing solutions fully integrate with EHRs. This reduces the workload, causes fewer errors, reduces missed follow-up appointments, speeds up payments, and offers a unified view of patient data in a few clicks. Claims data and medical charges automatically pass into the EHR, drastically cutting manual processes and duplicated data entry. As a result, your medical practice can focus on patient care while maintaining profitability.
Read also how to integrate telehealth module into EHR and guide on custom telemedicine software development.
If your EHR system lacks the functionality responsible for billing clients, you can integrate medical billing software into it. Usually, EHRs are secure systems that don’t allow adding random software with a click of a button. So, you would need to contact a software development vendor who has experience integrating medical systems to do this the right way.
How to develop a custom medical billing software from scratch
Building online software for medical/hospital bill processing is not difficult, but it requires proper planning. From the outset of your business and development process, you'll be making several key business and accounting decisions.
Gather a team
You'll have to decide if you want to hire in-house developers or freelancers or if your practice would benefit from outsourcing your software development. Regardless of what you choose, the team should be fully committed to supporting the project from start to finish. Every member of your development team should have a task, and every task should be defined and associated with a deadline.
Analyze your budget
Before you partner up with outsourced or in-house developers, you'll need to budget your expenses. What will the development cost be? What are your resources? Will you need support from external investors? Think these questions through before committing to anything.
Document your requirements
You need to be open about your requirements for developing a medical billing system. Depending on your business goals and overall vision, you may want to integrate some usual or innovative features to solve potential issues or provide extra value to your clients. Acknowledge and discuss them with your team.
Together, you should write all your requirements down in a separate document called ‘software requirements specifications.’ The specs should be very detailed, and you or team managers have to make sure the development process adheres to them.
Ensure integrations
Your medical billing software requirements need to include integrations with insurance providers to make it easy for you to verify your patients' insurance eligibility. Integrations with other software should also be on the list since it’s always easier to add another module or a third-party tool to extend your existing one than build an entire system from scratch.
Agree on the UI and UX design
Medical billing software contains a lot of information, so when designing its user experience, make sure to inform the user but not overload them with information. Also, pay attention to the navigation: since it will cover numerous items, the menu has to be intuitive. The readability of fonts and the color scheme also influence the software’s usability.

Choose a platform
Do you want a desktop or a mobile version? Maybe both? Will the mobile version be for Android and iOS or just one of them? Or perhaps all you need is a web-based medical billing software that will run equally well in the browser of a laptop and a tablet? Answering these questions will let you build software that’s most convenient for your practice.
Focus on security
Medical and insurance billing software processes confidential information, which makes data protection an important part of the development process. The application should schedule secure backups and provide data encryption while complying with data regulation and protection policies, such as HIPAA and GDPR.
Consider the storage
What type of information are you going to retrieve and store? Will you store it on your private server or in the cloud? How much storage do you need? These are all issues you will explore and decide with your development team at the beginning of your project.
Cost of medical billing software development
Depending on the approach you’re taking to build the solution, you can either outsource medical billing software development or build one in-house. A report by Grand View Research forecasts that the market size of medical billing outsourcing will continue to grow, while the share of in-house development will largely stay the same.
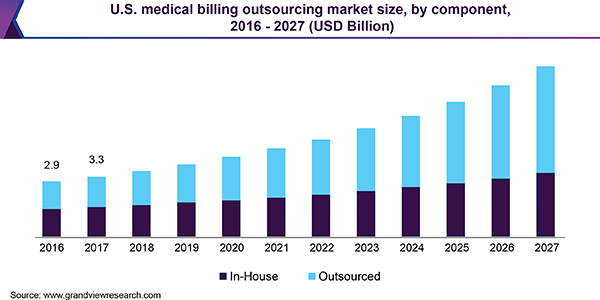
Most software development outsourcing vendors charge a rate per hour of work, but the cost of building medical billing and coding software will also depend on its features. The complexity and number of features you want to include will influence the development time and how many people you need to build the software.
As a rough estimate, you can expect to pay an outsourcing vendor around $50/hour (the exact rate will depend on the vendor, your location, and the complexity of the task). The testing and "post-release" maintenance of the billing application are also fundamental parts of the development process: remember to include them in your budget. Not all vendors offer post-support services after they've released an application. This means that you need to plan on subcontracting or hiring in-house to update the software and fix potential bugs.
If you opted to hire development staff in-house, you would need to do all the recruiting, onboarding, and maintenance of the new employees on your own. In that case, on top of paying the monthly salary, you should also add the hiring costs, paid vacations, and everything else a specialist needs to the bill. You will also have to pay for any additional tools like issue tracking software (e.g., Jira), software licenses, and cloud storage.
Demigos for customized billing software development
Automating bills and insurance claims through a cloud-based medical billing solution has numerous advantages. So, before jumping into building one for your healthcare business, make sure to partner up with a software provider who knows the tips and tricks of hospital billing software development.
Demigos is a software development vendor who lives by the principles of innovation, collaboration, and security. We work with clients from early research and idea generation to product launch, maintenance, and promotion. Our team has expertise in software engineering with a focus on HealthTech.
Contact Demigos to learn more about how we can help you build the medical billing and coding software that's right for your organization.






